Key takeaways
- There are a range of private cover options for the common sterilisation and sterilisation reversal procedures.
- Simple procedures like vasectomies are covered under many Bronze health policies.
- More complex procedures like hysterectomies may require a top-tier plan.
Health insurance policies for sterilisation
Below you'll find a selection of Finder partners that cover sterilisation, and the minimum policy tier that covers the treatment. All have a two-month waiting period. All prices are based on a single individual with less than $101,000 income and living in Sydney.
Finder survey: What are the main reasons Australians have hospital insurance?
| Response | |
|---|---|
| To avoid public surgery waiting lists | 44.76% |
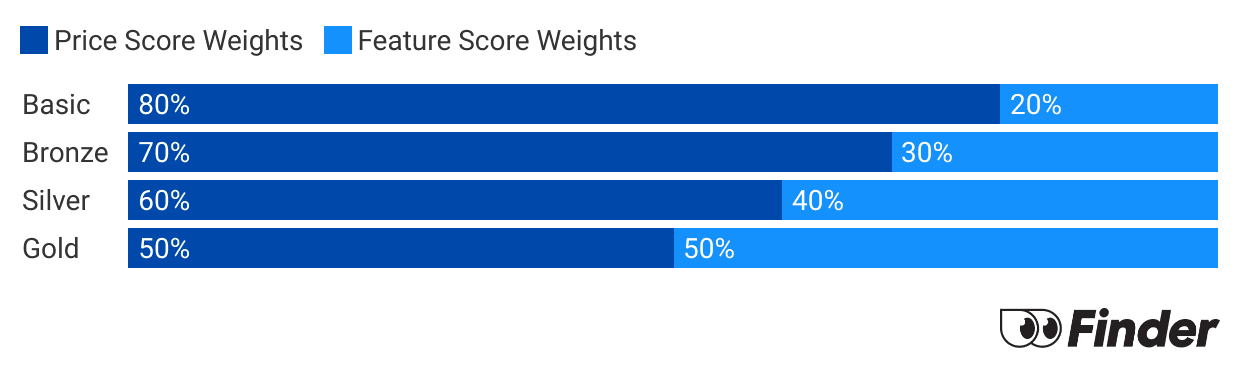
Finder Score - Hospital cover health insurance
Each month we analyse our hospital insurance products and rate each one on price and features. What we end up with is a nice round number out of 10 that helps you compare hospital cover a bit faster.
Before we start scoring, we need to make sure we're comparing like-for-like. Just as it doesn't make sense to compare a bicycle with a Ferrari, it doesn't make sense to compare basic hospital policies to top-tier Gold policies. Each policy is given a price score and feature score. These are then combined to determine each policies's Finder Score.
What are the main types of sterilisation available?
In general, if someone never wants to have children then sterilisation can be an effective option. The two most widely-used methods of voluntary sterilisation are:

Vasectomy
A vasectomy involves a man having his vas deferens severed or sealed. This prevents him from impregnating women with no major impact on sexual functioning. The procedure does not require hospitalisation and can usually be performed in 30 minutes or less.

Tubal ligation
This procedure involves the surgical severing and/or blocking of a woman's fallopian tubes. This prevents the passage of eggs to the uterus and renders pregnancy near impossible.
In Australia, it is illegal to undertake either of these procedures on persons under the age of 18 unless it is a clear medical necessity. Needless to say, no health insurance will cover illegal procedures.
Must read
If you think you might want to undo your vasectomy or tubal ligation in the future, then do not get it at all.
Reversal surgery does not guarantee that you will recover full functionality, and in some cases will be completely ineffective. The high costs and indeterminate success rates of sterilisation reversal procedures mean that private health funds will typically only cover them as on more comprehensive policies.
How does health insurance handle contraceptive surgery?
Private health funds will cover vasectomies, tubal ligation and hysterectomies in varying ways, depending on the level of cover you have purchased and the conditions of the policy. Things to consider are:
- Your level of cover. Because sterilisation is an elective procedure, vasectomies and tubal ligation are typically covered under higher-tier hospital policies. Check your health insurance policy's Product Disclosure Statement (PDS) or contact your fund to find out if your policy covers it.
- Your hospital cover. Vasectomies do not usually require hospitalisation, but tubal ligation does and hysterectomies in particular require spending several days in hospital. Hospital stays will incur additional costs. To find out how a private health fund covers these and the limits which may apply, look at the hospital cover section of the policy. It is possible that your health fund will cover the surgery itself, but won't cover the hospital stay and related costs.
- What sterilisation covers. Sterilisation typically refers to tubal ligation and vasectomies. Sterilisation is the term to look for if you want a private health fund to cover your contraceptive surgery, and it is a good idea to familiarise yourself with the terms and conditions surrounding it.
- What gynaecological services covers. In both the hospital and general cover sections you may find that a policy includes gynaecological services. Typically this refers only to medically necessary services, like emergency hysterectomy, and not elective ones like tubal ligation.
- What fertility and infertility services mean. Fertility and infertility services, although related to sterilisation, are not connected to the contraceptive surgeries on offer and do not cover vasectomies or tubal ligation (which are sterilisation) or hysterectomies (which is a gynaecological service). However they do refer to vasectomy or tubal ligation reversal surgery, which is a procedure to undo sterilisation.
Can't I just get these types of medical service under Medicare?
You can. Because vasectomies and tubal ligation are not emergencies and Medicare offers relatively good benefits for them.
So, it's not usually worth choosing a fund on the basis of whether or not they cover these. However, going private may still be worth considering if:
- You only want to see a particular practitioner for your vasectomy or tubal ligation.
- You don't want to wait for a bulk-biller to fit you in.
- You are considering an elective hysterectomy for reasons such as a family history of cervical cancer.
How do I claim sterilisation services on health insurance?
To claim a vasectomy or tubal ligation with a private health fund:
- Make sure your chosen doctor is approved by the health fund.
- Book an appointment and confirm that they work with your fund.
- Pay them in a way approved by the insurance plan. This may be by simply swiping a health fund membership card, giving them your details, or paying up-front and then claiming it back later.
Claiming a hysterectomy can be more complicated as it depends on your reason for having the procedure and the methods used by the surgeon.
Bottom line
Having a vasectomy or tubal ligation procedure is easy and relatively inexpensive, but it should also be considered very carefully first. Covering sterilisation with public or private health insurance is simple, but undoing it can be much more complex and expensive.
- Extras only: $53
- Basic: $90
- Bronze: $144
- Silver: $184
- Gold: $285
Frequently asked questions
More guides on Finder
-
Health insurance for kidney dialysis
Dialysis treatment for Chronic Kidney Disease (CKD) is covered by Medicare and private health insurance, but which offers the best cover?
-
Health insurance for podiatry
Find out the steps needed to find adequate cover, and give you an assurance that you won’t have to pay the full cost of your podiatric surgery.
-
Health insurance for grommets
Want to get health cover for grommets? Find out how private health insurance and Medicare costs compare and what you'll be covered for. Choose the option that suits you best.
-
Health insurance for endometriosis
Find health insurance for endometriosis. Compare Medicare and PHI options and see how affordable cover can be.
-
Health insurance for hernia surgery
Think you may need hernia surgery? See what's involved.
-
Health insurance for hip replacement surgery
Think you may need hip surgery in the future? Compare your options for public and private treatment.
-
Health Insurance for Joint Fluid Replacement Injections
What are joint fluid replacement injections and are they covered by private health insurance? Find out here.
-
Health insurance for travel and accommodation expenses
Will private health insurance provide cover when you need to travel far from home and stay overnight to access medical treatment? Find out here.
-
Health insurance for prostheses
There are more than 10,000 prosthetic devices that can be covered through private health insurance. Here's how to identify if you're covered.